
Behavioral Health Billing RCM: The Complete Guide to Stopping Claim Denials and Fixing Your Cash Flow
Table of Contents
You just spent a grueling hour helping a patient navigate a severe mental health crisis. You did your job perfectly. But 30 days later, the insurance company denies your claim. You provided the care, yet your practice gets paid absolutely nothing. If you run a therapy clinic or addiction center, mastering your behavioral health billing rcm is the only way to keep your doors open. It is not just administrative paperwork; it is a constant fight to collect the money you actually earned.
Why is this happening right now? Payer rules are getting tighter, and mental health claims face a level of scrutiny that standard medical clinics never deal with. Insurance companies actively look for tiny mistakes. A missed prior authorization, a mismatched diagnosis code, or a simple typo on a demographic form will instantly halt your cash flow. Most independent practices simply cannot survive a 20% denial rate in today’s economy.
We are going to plug the holes in your financial pipeline right now. This guide will show you exactly how to rebuild your internal processes, catch fatal claim errors before the patient even arrives, and secure predictable revenue.
The Reality Check: Why Your Claims Are Actually Failing
Over the past few years, I have audited massive revenue cycles and built systems like the AI Practice Acquisition System (APAS) to help billing operations scale. I dig into the data daily. When I handle the operational transition for multi-provider groups—like taking over the digital footprint for entities similar to Indiana Neurology and Pain Center—I see the same exact failure point. Claims do not fail at the clearinghouse. They fail in the therapist’s chair.
Here is the truth. The insurance company does not care about your patient’s clinical breakthrough. They only care about the CPT code. I recently watched a mid-sized clinic bleed thousands of dollars for a simple reason. The therapists wrote notes for 45-minute sessions, but the billing staff kept slapping 60-minute codes on the claims. The payer audited them, caught the mismatch, and demanded their money back.
If your clinical notes do not perfectly match your billing software—minute for minute—you are inviting a massive CMS clawback. Your financial team and your clinical staff must speak the exact same language. You cannot fix a revenue cycle problem if your therapists do not understand how they get paid.
Standard Medical Billing vs. Mental Health Revenue Cycles
Standard medical billing makes sense. A patient comes in with a broken wrist. The doctor takes an X-ray, puts on a cast, bills the code, and gets paid. Mental health is entirely different. Psychiatric care is subjective, ongoing, and requires constant proof.
Insurance companies obsess over medical necessity. They want concrete proof detailing exactly why a patient needs weekly therapy and how long the treatment will last. If your clinical documentation does not tell that specific story, the claim dies.
The Time-Based Coding Trap
One of the worst traps in this specialty is time-based coding. Most therapy codes require an exact number of face-to-face minutes according to the official CPT guidelines published by the American Medical Association (AMA). If you bill a 60-minute session (CPT 90837) but only talk to the patient for 47 minutes, you just committed billing fraud in the eyes of the payer. If they audit you, you lose. Your strategy must include hard, non-negotiable internal audits of session times.
| CPT Code | Description | Typical Payer Rules | The Reason You Get Denied |
|---|---|---|---|
| 90791 | Psychiatric diagnostic evaluation | Usually limited to one per year. | You billed it twice without getting special authorization first. |
| 90834 | Psychotherapy, 45 minutes | Must be between 38-52 minutes. | The session time in your notes does not match the 90834 code. |
| 90837 | Psychotherapy, 60 minutes | Highly audited. Needs 53+ minutes. | You failed to document the medical necessity for the extra time. |
| 90847 | Family psychotherapy | The patient must be present. | You billed it when the primary patient was not in the room. |
| 90853 | Group psychotherapy | Strict limits on group size. | You put too many people in the group for the payer’s rules. |
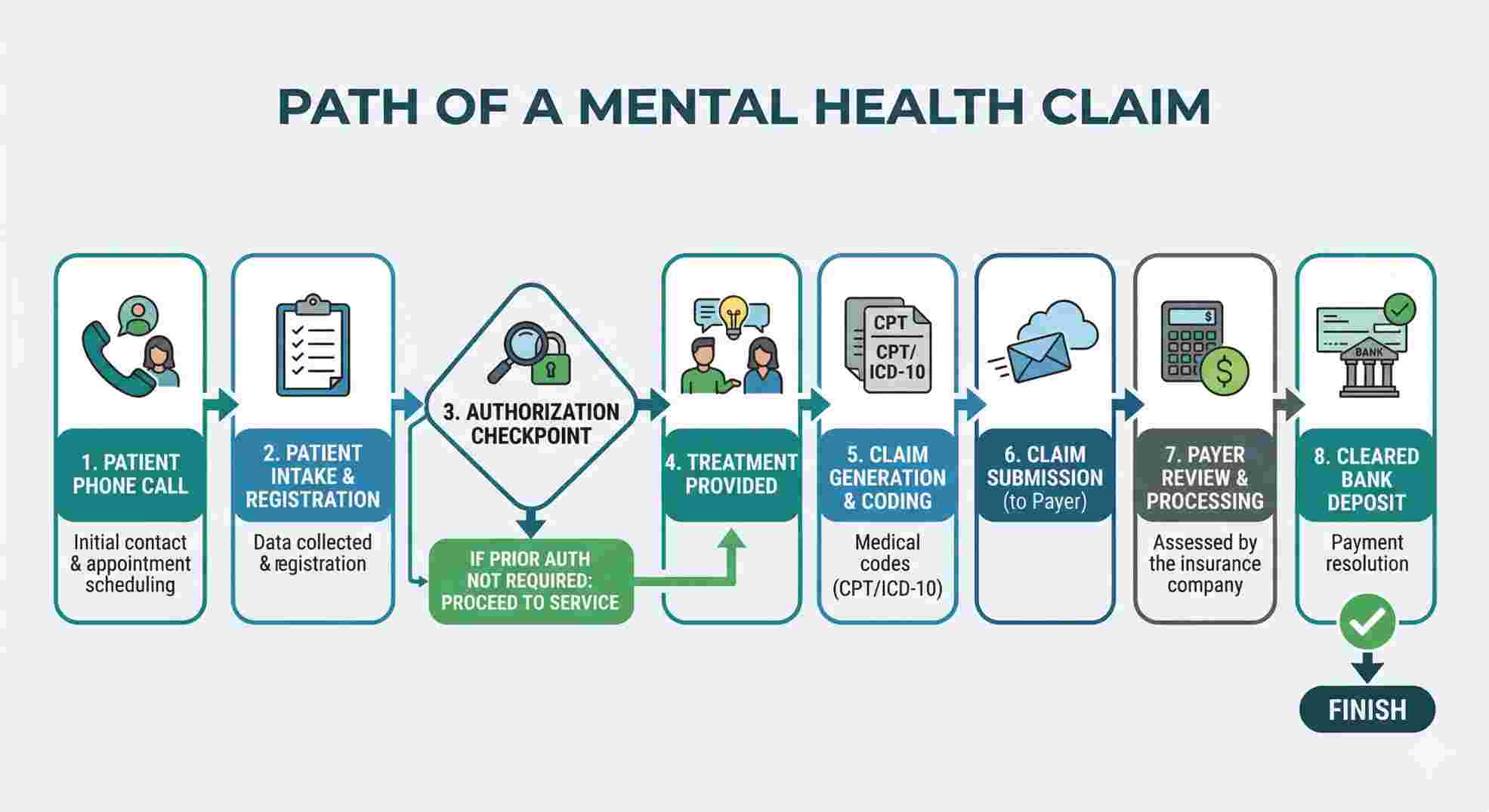
Stop Chasing Unpaid Claims: The Front-Desk Fix
Most practice owners spend all their time trying to fix denied claims. That is a losing game. The secret to a highly profitable clinic is stopping the denial before the patient ever walks through your front door.
Over 70% of claim denials happen because the front desk made a mistake. You need a strict policy starting tomorrow morning. Nobody sees a therapist until your staff verifies active insurance coverage and secures the prior authorization. You also must check for carve-outs. Often, a patient has Blue Cross for their physical health, but a completely different company handles their mental health benefits. If you send that claim to Blue Cross, you just wasted three weeks waiting for a rejection letter. Secure the money upfront.
Why Your Behavioral Health Billing RCM Strategy Fails Without the Right Software
You cannot run a modern clinic on paper charts and sticky notes. You need technology that actually works. But generic medical software will fail you. You need tools built explicitly for psychiatric and therapeutic workflows.
When you shop for practice management software, demand deep EHR integration. Your clinical notes must generate the billing codes automatically. If your therapist types notes into one system and your biller types codes into another, someone will make a typo. That typo will cost you $150.
Your tech stack needs to do the heavy lifting. It should flash a red warning when a patient’s authorization expires. It should tell the front desk exactly how much copay to collect.
| Software Feature | What It Actually Does | The Impact on Your Cash Flow |
|---|---|---|
| Automated Eligibility Checks | Pings the insurance company before the visit. | Kills front-end demographic denials instantly. |
| Authorization Tracking | Counts down approved therapy sessions. | Stops you from giving away free, unbillable therapy. |
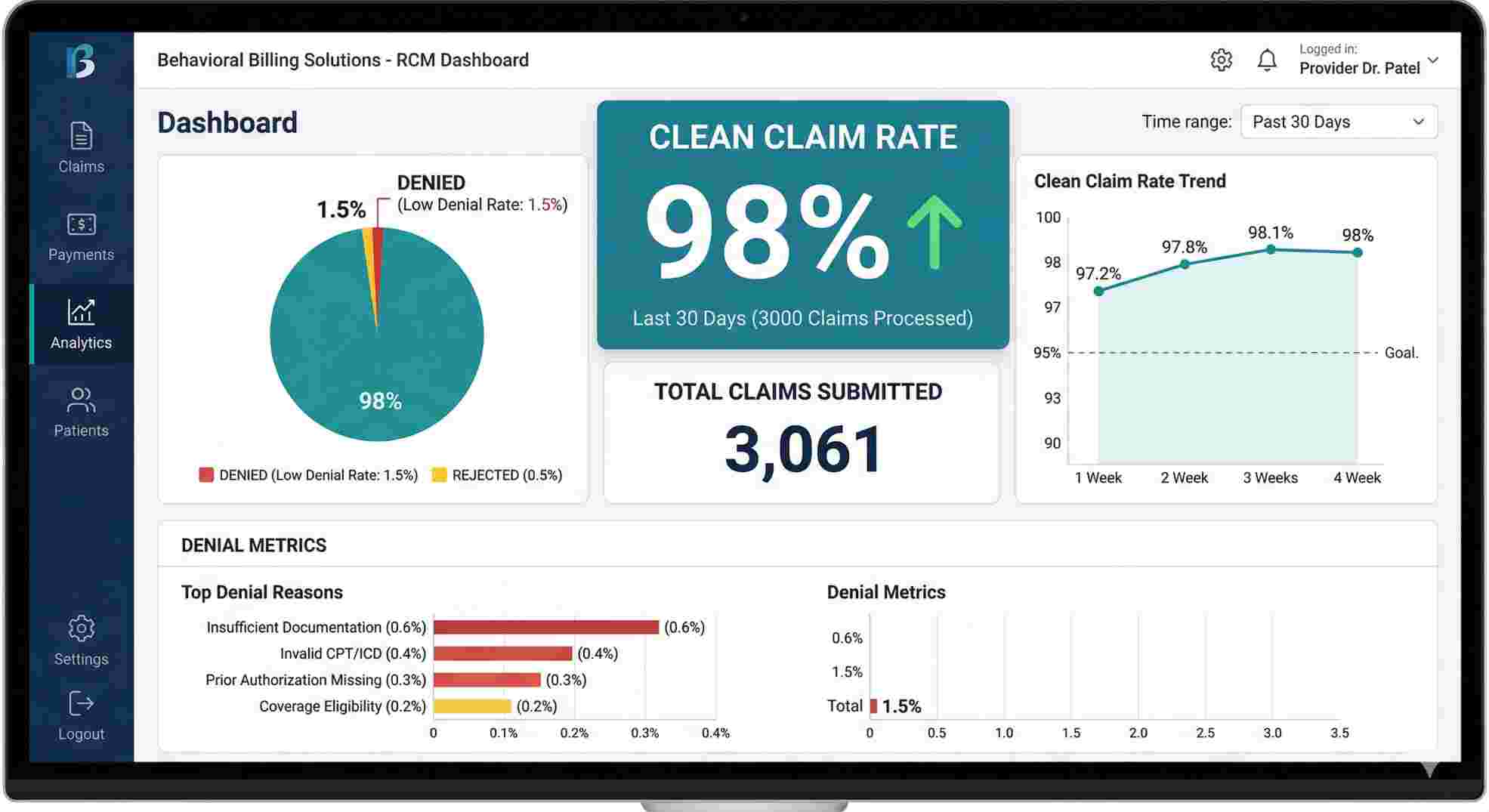
| Custom Claim Scrubbing | Catches your coding mistakes before submission. | Pushes your clean claim pass rate above 95%. |
| Integrated Patient Portal | Lets patients pay their bills online via phone. | Gets you paid faster by patients with high deductibles. |
| Real-Time Analytics | Shows exactly how much money is stuck in A/R. | Gives you total control over your financial health. |

Building an In-House Team vs. Outsourcing Your Revenue Cycle
As your patient list grows, you hit a wall. Do you hire more internal billers, or do you outsource to an external agency? This is the most important financial decision you will make this year.
Running an internal billing team is expensive. You pay salaries, payroll taxes, and health benefits. You spend hours training them on new Medicare rules. And if your lead biller quits on a Tuesday, your cash flow stops on Wednesday.
Outsourcing gives you specialized experts. These agencies already know how to fight Optum and Magellan. They know the exact appeal codes to use. This is exactly why we built RCM Finder’s Behavioral & Mental Health Billing Services. The platform connects your clinic directly with vetted billing partners who deliver precise operational solutions, completely removing the massive financial overhead and daily headache of internal HR issues.
| Factor | In-House Billing Staff | Outsourced RCM Services |
|---|---|---|
| Daily Control | You direct every task and set the daily schedule. | You rely on their monthly reporting and trust the process. |
| Financial Cost | High fixed costs (salaries, software seats, benefits). | Variable costs (you only pay a percentage of what they collect). |
| Growth Speed | Slow. You have to interview and train new people. | Instant. They add more staff to your account as you grow. |
| Industry Knowledge | Limited strictly to what your current employees know. | Access to massive teams who only do specialized billing. |
| Business Risk | High. If staff get sick, claims sit unworked. | Low. Your billing continues running every single day. |

The Nightmare of Addiction Treatment Billing
Substance abuse treatment is easily the hardest specialty to bill. These facilities move patients through different levels of care rapidly. A patient goes from medical detox, to residential care, to an intensive outpatient program (IOP).
Every single step down requires a brand new prior authorization. It requires different CPT and revenue codes. Insurance payers fight addiction claims aggressively. If your therapist writes a note that does not explicitly prove the patient still needs residential care, the insurance company will deny the claim and refuse to pay for the bed.
To survive this, you need a daily utilization review. Your clinical director and your head biller must talk every single morning. They must confirm that every patient in a bed has an active authorization on file. If they do not, you are losing money by the hour.
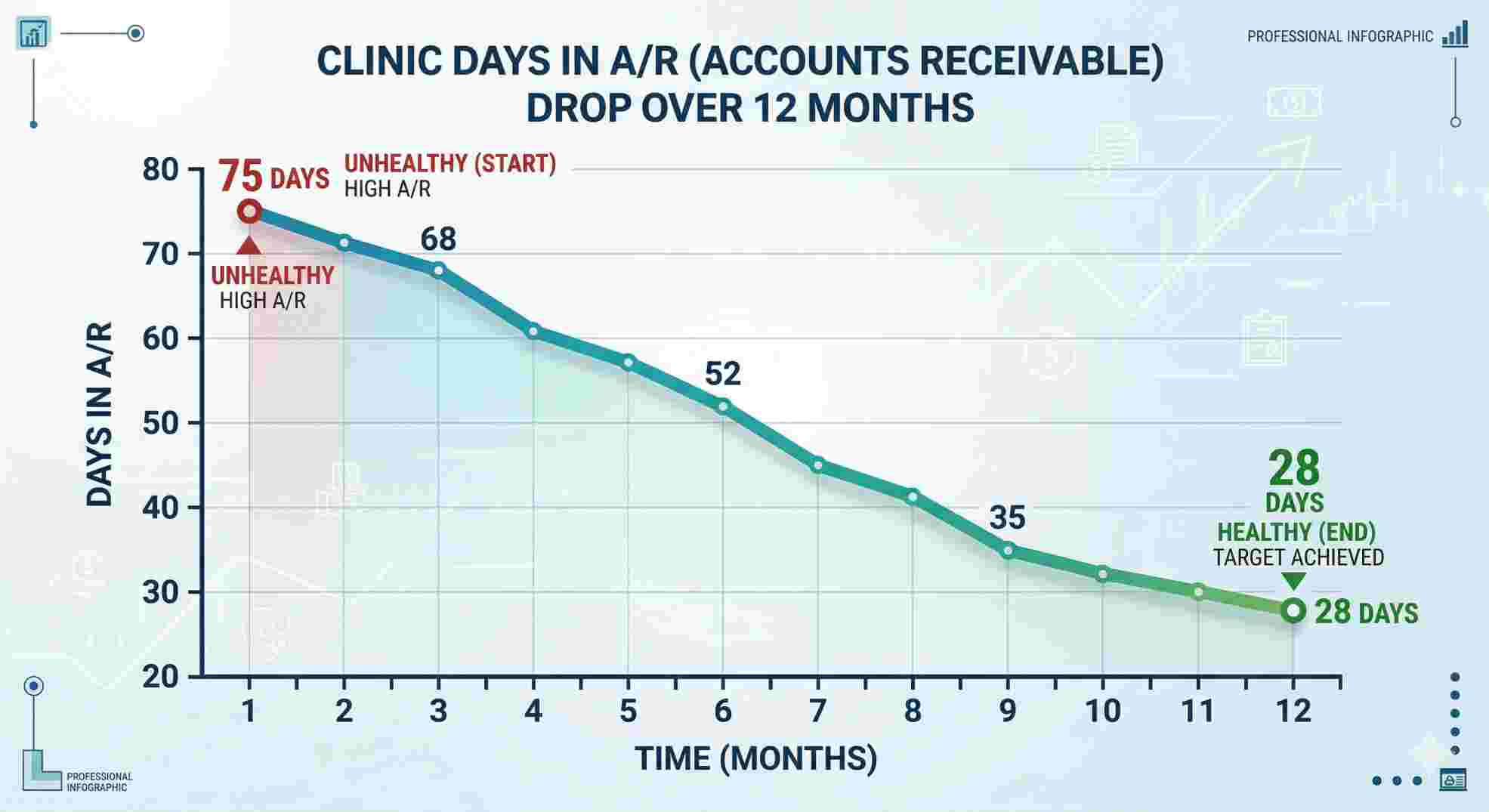
Accounts Receivable Management: Go Get Your Money
Sending the claim out is easy. Getting the money back is the hard part. A/R is the money insurance companies owe you, but haven’t paid yet.
A strong clinic keeps its days in A/R under 35 days. If you have claims sitting unpaid for 90 days, you are failing. You are giving multibillion-dollar insurance carriers a free loan. You have to attack your aging reports.
Never start at the top of the A/R list. Start with the oldest, highest-dollar claims first. Insurance companies enforce strict “timely filing” limits. If you wait too long to fix a denial, the window closes. You lose the right to appeal, and you have to write off the balance. Instruct your team to hunt down the old, high-value claims before they expire.
Stop Leaving Your Money on the Table
You do not have the luxury of running sloppy administrative processes anymore. The margins in healthcare are shrinking, and payer audits are only getting more aggressive. Every denied claim is money stolen directly out of your clinic’s operating budget.
You have to take control back. Build an ironclad front desk. Force your clinical staff to understand how time-based coding works. Invest in software that actually talks to your EHR. Whether you hire an aggressive internal team or hand the keys to an expert agency, the goal is the same. Stop fighting the same old denials. Take control of your behavioral health billing rcm today, protect your revenue, and get back to focusing on the patients who need you.
Ready to Stop the Revenue Leaks? Let’s Look at Your Data.
You did not endure years of rigorous medical training just to argue with a stubborn insurance rep over a therapy code. It drains your energy. Every hour you spend fighting a denied claim is an hour stolen from a patient who desperately needs your help. It is time to hand that massive administrative burden over to specialists who actually know how to win these financial fights.
Let our dedicated Behavioral & Mental Health Billing Services team aggressively audit your revenue cycle, stop the cash leaks, and secure the money your facility actually earned. Stop leaving your hard-earned revenue in the hands of insurance companies.
Secure a meeting with our dedicated experts today. We will audit your current workflow, evaluate your exact denial reasons, and show you exactly how to get the absolute most out of this highly specific specialty. Stop wondering where your money went. Start the conversation right now.
Your Immediate Action Plan
Do not wait until next month to fix these leaks. Implement these structural steps right away:
- Phase 1: Front Desk Fortification: Your front desk is your primary shield. Train them to intercept invalid insurance before the session starts.
- The Strict 48-Hour Rule: Every single patient must have their full benefits checked at least two days prior to their appointment. No exceptions.
- Conduct Daily Staff Audits: Review your front desk’s verification logs at the exact end of every shift to ensure absolute compliance across the board.
About the Author: Awais Afzal
Awais Afzal is an experienced healthcare entrepreneur, content strategist, and technical SEO expert. With a deep specialization in US healthcare Revenue Cycle Management (RCM) and medical billing compliance, Awais builds and scales digital tracking systems and operational infrastructures for medical practices. He has successfully managed comprehensive digital transitions for multi-provider groups like Indiana Neurology and Pain Center, and leads the development of high-level growth frameworks including the AI Practice Acquisition System (APAS). His work bridges the gap between complex CMS compliance guidelines and profitable clinical operations.
Schedule Zoom Meeting
You did not endure years of rigorous medical training just to argue with a stubborn insurance rep over a therapy code. It drains your energy. Every hour you spend fighting a denied claim is an hour stolen from a patient who desperately needs your help. It is time to hand that massive administrative burden over to specialists who actually know how to win these financial fights. Let our dedicated Behavioral & Mental Health Billing Services team aggressively audit your revenue cycle, stop the cash leaks, and secure the money your facility actually earned. Stop leaving your hard-earned revenue in the hands of insurance companies. Secure your meeting today and let us fix your cash flow for good.

