
Mastering the 90832 CPT Code Description for Better Reimbursement
Table of Contents
You finish a session, check the clock, and realize you are in that weird gray area. You spent 25 minutes with a client. Maybe 28. It definitely wasn’t a full hour, but it wasn’t a brief check-in either. Now you are staring at your billing software, trying to recall the exact 90832 cpt code description to figure out if you can actually bill for this time.
This is where understanding the rules saves you. If you don’t understand this code, you are likely leaving money on the table every single week. Or worse, you are billing incorrectly and putting a target on your back for an audit.
Insurance companies are watching time-based codes like hawks right now. Many therapists default to the standard 45 or 60-minute codes just because it feels “safer,” often under-coding out of fear. But precision—a core principle of The Real Truth About Coding and Billing for Mental Health Services—isn’t just about compliance; it’s about maximizing your revenue stream without looking over your shoulder. You need to know exactly when a short session is valid and how to prove it.
The fix is simple. You just need to master the time rules for the 30-minute session. I’m going to walk you through the specifics—from the exact minutes you need on the clock to the words you need in your paperwork.

The “16-Minute Rule”
Here is the one thing you need to remember if you forget everything else: The 16-Minute Rule.
A lot of providers think CPT 90832 requires exactly 30 minutes of face-to-face time. It does not.
According to standard CPT guidelines for psychotherapy, the 90832 time range starts the second you hit 16 minutes. The actual window is 16 to 37 minutes.
If you handle a crisis call that lasts 18 minutes? That’s a 90832.
If you have a session that runs 35 minutes? Still a 90832.
Knowing that the floor is 16 minutes and the ceiling is 37 minutes changes how you schedule. It gives you freedom.
What Is the 90832 CPT Code Description?
Let’s look at the actual text. The 90832 cpt code description defines the service simply as: “Psychotherapy, 30 minutes with patient and/or family member.”
It sounds basic, but it covers a lot of ground. This is your designated code for focused, shorter therapy sessions. It isn’t an intake (that’s 90791). It isn’t a standard hour (that’s 90837). It is for treatment that gets straight to the point.
When you read the 90832 cpt code definition, you realize it doesn’t care about your modality. You can do CBT, solution-focused work, or supportive counseling. It also doesn’t matter if you are talking to the patient alone or with a family member present. The only things that count are the time on the clock and the face-to-face interaction.
Just remember: this code is for psychotherapy. If you are a prescriber doing medication checks, you are likely looking at E/M codes with add-ons. But for therapists, social workers, and counselors, the 90832 cpt code description is the bread and butter of short-form treatment.
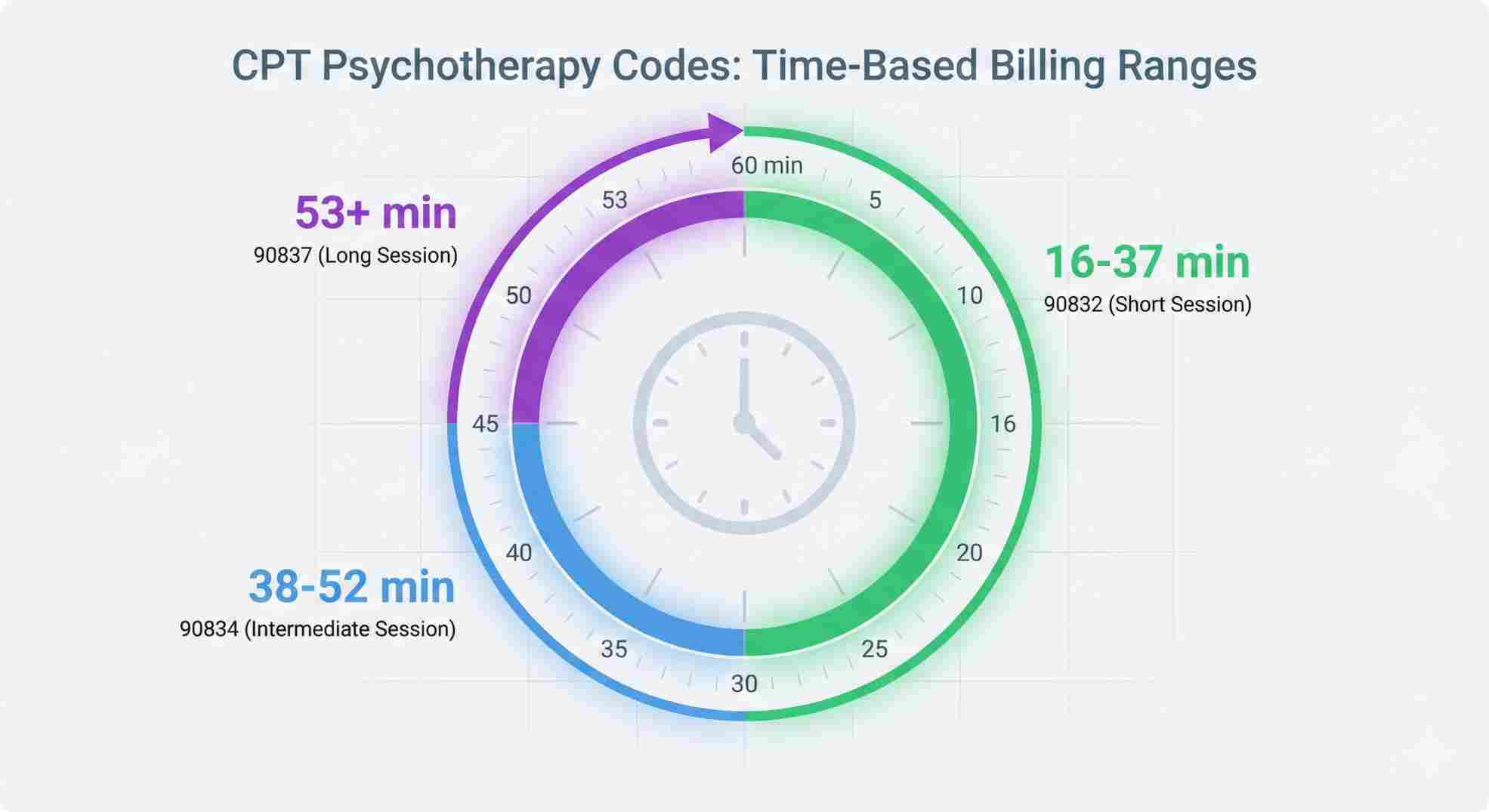
The Critical Time Rule: When to Use 90832
Time is strict in billing. You can’t round up. If your session was 15 minutes, you can’t bill this code. You honestly can’t bill a therapy code at all for that (it falls into unbillable time or a different category depending on your license).
Understanding the 90832 time range is what keeps your revenue safe.
The Midpoint Rule
CPT codes work on averages. The code says “30 minutes,” but that is just the midpoint. You qualify for the code once you pass the midpoint of the previous block.
Here is how the 90832 cpt code description fits with the other codes you use.
| CPT Code | Official Description | Minimum Time | Maximum Time | Best Used For |
|---|---|---|---|---|
| 90832 | Psychotherapy, 30 minutes | 16 minutes | 37 minutes | Quick check-ins, kids, schools. |
| 90834 | Psychotherapy, 45 minutes | 38 minutes | 52 minutes | Standard weekly sessions. |
| 90837 | Psychotherapy, 60 minutes | 53 minutes | Unlimited* | Trauma work, deep processing. |
*Most insurance plans cap 90837 at 60 minutes for payment.
If you do 37 minutes of work, you must use the 90832 cpt code description. The moment you hit minute 38, you bump up to 90834. This hard cutoff is why you have to document your start and stop times exactly.
Why Schedule a 30-Minute Session?
You might be thinking, “Why would I bother with 30-minute sessions?” Most of us live by the 50-minute hour. But the cpt code for 30 minute psychotherapy is actually a really useful tool.
Real World Examples
There are times when a short session is actually better clinically.
- Kids: Try getting a 6-year-old to sit for 50 minutes. It’s a nightmare. 30 minutes of play therapy is often perfect.
- Crisis Checks: A client is panicking on a Tuesday but sees you Friday. A 20-minute video call to calm them down fits the 90832 cpt code description perfectly.
- Hospital Work: If you work inpatient, you are often seeing patients at bedside for 20 minutes.
- Tapering Off: A client is doing well and just wants a monthly check-in.
Using the right cpt code for 30 minute therapy session lets you serve these clients without blocking a full hour on your calendar. It makes your schedule more flexible.

Documentation: How to Audit-Proof Your Notes
If it isn’t written down, it didn’t happen. That is the rule. When you use the 90832 cpt code description, your notes have to back it up.
Auditors look for “upcoding”—billing 45 minutes when you only did 30. But they also catch people who didn’t write down the time at all.
What You Need in the Note
To get paid for 90832, your note needs these four things:
- Exact Times: Don’t write “30 mins.” Write “10:00 AM – 10:32 AM.” This proves you hit the 90832 time range.
- Modality: What did you do? (CBT, talk therapy, etc.)
- Focus: What problem are you working on?
- Result: How did the patient react?
A Simple Note Template
“Patient met for scheduled psychotherapy. Start: 2:00 PM. End: 2:28 PM (28 mins total). Discussed anxiety about new job. Used CBT to challenge negative thoughts. Patient felt calmer by end of session. Will resume next week.”
That’s it. That note is solid. It justifies the cpt code for 30 minute therapy session and matches the 90832 cpt code description.
What Does It Pay?
Let’s talk numbers. How much does the 90832 cpt code description actually put in your bank account?
Usually, 90832 pays about 70% of what a 45-minute code pays. It sounds like less, but do the math. If you see two patients for 30 minutes each in one hour, you usually make more than seeing one patient for 60 minutes.
| Payer | CPT 90832 (30 mins) | CPT 90834 (45 mins) | CPT 90837 (60 mins) |
|---|---|---|---|
| Medicare | $60 – $75 | $85 – $105 | $110 – $135 |
| Medicaid | $40 – $60 | $60 – $80 | $80 – $100 |
| Private Plans | $50 – $90 | $75 – $120 | $90 – $150 |
*Note: These are estimates. Your contract determines the exact rate.*
Two 90832s could net you $140/hour. One 90837 might only net you $120. Efficiency pays.
Telehealth and Add-Ons
Telehealth is here to stay. Does the 90832 cpt code description change on Zoom?
No. The description is the same. But the way you put it on the claim form is slightly different.
Modifiers
For a video session, you almost always need a modifier so the insurance company knows you weren’t in the same room.
- 95: This is the standard for “Synchronous Telemedicine.”
- GT: Some older systems or specific payers still want this one.
You list it as 90832-95.
Interactive Complexity
Sometimes a 30-minute session is really hard work. Maybe there is a language barrier, or a kid is screaming, or you are using play equipment. In those cases, you can bill the 90832 cpt code description PLUS code 90785 (Interactive Complexity). This tells the payer, “This was a difficult session,” and they usually pay a bit more.
| Code/Modifier | What It Is | What It Does |
|---|---|---|
| 95 | Telehealth | Shows it was video. |
| GT | Telehealth (Legacy) | Shows it was video (old style). |
| 90785 | Interactive Complexity | Pays more for difficult communication. |
| HE | Medicaid Program | Required by some Medicaid states. |

Where People Mess Up (Don’t Do This)
I see claims get denied all the time. Usually, it is a simple mistake with the 90832 cpt code description.
1. Confusing it with E/M
If you are a doctor doing med management and therapy, you don’t bill a standalone 90832. You bill an E/M code plus an add-on therapy code. 90832 is for therapy only.
2. Bad Timing
If your note says “15 minutes,” you won’t get paid. The floor is 16 minutes. Period.
3. Double Dipping
You generally can’t bill a 90832 and a 90834 for the same patient on the same day. Insurance sees that as “unbundling.” If you see a patient twice in one day, add the time together and bill one big code (like 90837). It’s safer.

Wrap Up
Billing doesn’t have to be hard. Once you understand the 90832 cpt code description, you can treat your clients the way they need to be treated without worrying about your paycheck. Whether it’s a restless kid or a quick check-in, this code is a tool you should be using.
Just stick to the rules: 16-37 minutes. Document your times. Keep the focus on therapy.
Don’t let the paperwork scare you. Use the 90832 cpt code description the right way, get paid for your time, and get back to helping people.
FAQs About Mastering the 90832 CPT Code Description
Can I use 90832 for family therapy?
Does 90832 work for phone calls?
My session was exactly 37 minutes. Which code do I use?
Can 90832 be an intake?
How many times a week can I bill this?
Schedule Zoom Meeting
Your focus should be on patient outcomes, not on chasing denied claims or deciphering complex coding guidelines. Every hour you spend fighting with insurance companies is an hour taken away from the care your facility provides. Don’t let administrative burdens throttle your revenue or burnout your staff. By outsourcing your revenue cycle to specialists who understand the nuances of the industry, you ensure your facility is paid for every minute of care provided. Streamline your practice today with our dedicated Behavioral & Mental Health Billing Services and reclaim the time you need to help your patients heal.

